|
8/17/2023 0 Comments Body fluid compartments dunnet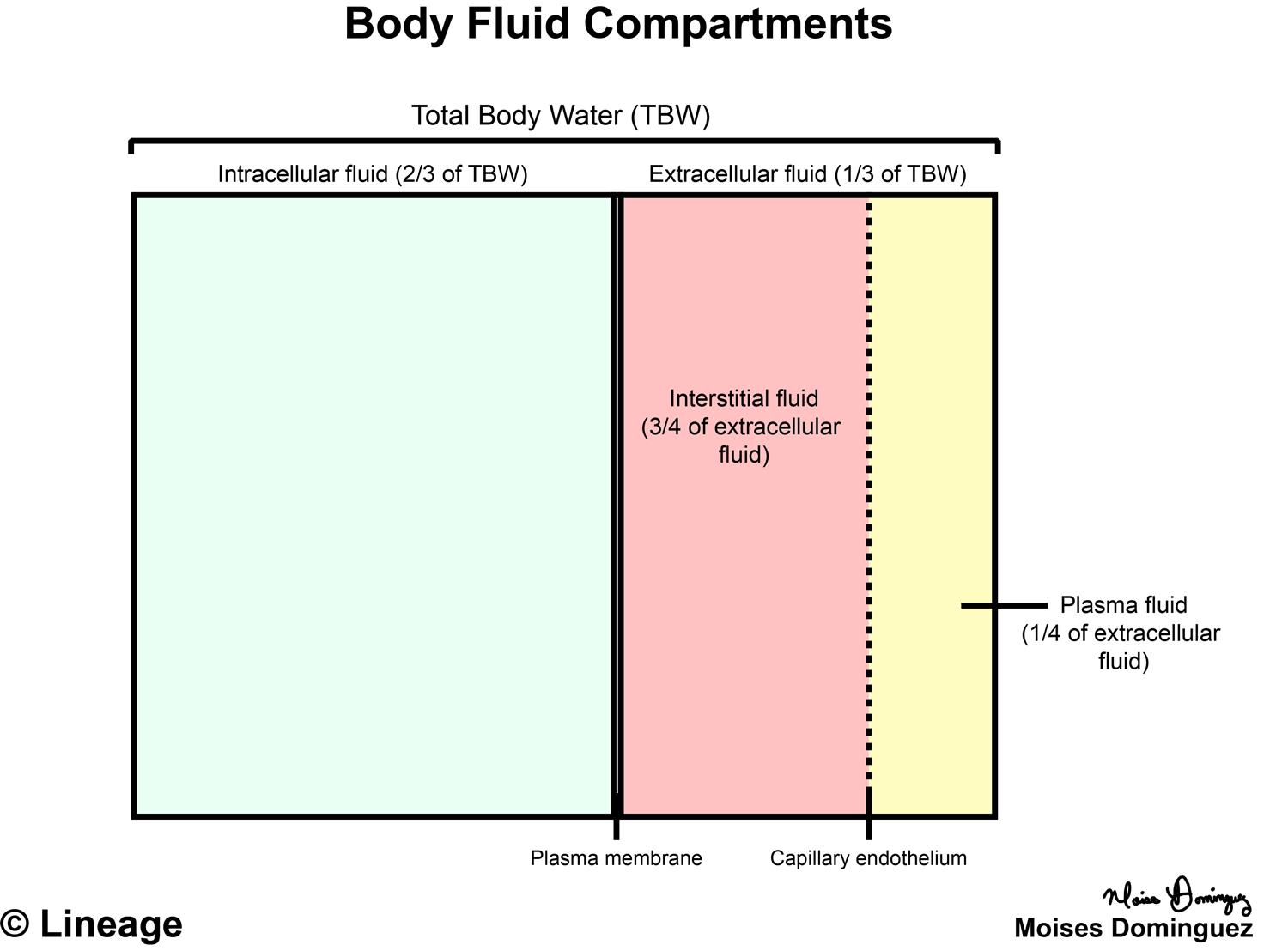
This was continued until achievement of 40 mmHg mean arterial blood pressure.  
Hemorrhagic shock (HS) was achieved with blood withdrawal at a maximum rate of 1 ml/min, from the femoral artery in a syringe pretreated with 8 units of heparin in 0.8 ml saline. The time-line for the experimental protocol is depicted in figure 1. Hemorrhagic shock and resuscitation model The femoral artery was cannulated with PE-50 tubing for blood withdrawal and the femoral vein for resuscitation. The right carotid was cannulated with PE-50 tubing for blood pressure monitoring with a pressure transducer (Digi-Med Signal Analyzers, Louisville, KY). Surgery was performed after loss of blink and withdrawal reflexes. Body temperature was maintained at 37 ± 0.5☌ with a rectal probe and a servo-controlled heating pad. Anesthesia was induced with intraperitoneal pentobarbital (60 mg/kg), and supplemental subcutaneous injections (20% the original dose) were given as needed to maintain a surgical plan of anesthesia. All animal and experimental interventions were performed under standard aseptic conditions. Animals were acclimated for 1 to 2 weeks before experimental use, during which time each animal received 15 g of rat food per diem and water ad libitum, except for the night before the experiment. Indianapolis) were used in the experiments. The Institutional Animal Care and Use Committee and Biohazard Safety Committee at the Louisville Veterans Affairs Medical Center approved the research protocol. For this reason, the present study was conducted to characterize the potential time dependency of neutrophil extravasations and sequestration and the possible modulation of neutrophil kinetics by adjunctive DPR from HS in rats.Īnimals were maintained in a facility approved by the American Association for Accreditation of Laboratory Animal Care. Thus, it is likely that intravital microscopy of the intestinal wall (terminal ileum) is not sensitive to visualize neutrophil extravasations because of the relatively thick tissue for Trans-illumination. In addition, regardless of the resuscitation regimen utilized, no white blood cell migration and extravasations were observed in our model. Conversely, no decrease in white blood cell-endothelium interaction was observed in rats subjected to hemorrhagic shock and resuscitated with conventional resuscitation alone or with conventional resuscitation plus adjunctive DPR. This vasodilation was associated with a marked increase in local blood flow and a significant decrease in the white blood cell-endothelium interaction. However, in a recent intravital microscopy study of the terminal ileum we have confirmed that topical intraperitoneal application of a glucose-based clinical peritoneal dialysis solution in naive rats produced an instantaneous and generalized vasodilation at all intestinal microvascular levels. DPR improves splanchnic and distal organ blood flow, promotes early fluid mobilization and markedly decreases the gut-derived exaggerated systemic inflammatory response and therefore results in a remarkable improvement in survival. DPR utilizes intraperitoneal instillation of a glucose-based clinical peritoneal dialysis solution into the peritoneal cavity as an adjunct to conventional intravascular fluid resuscitation. However, none of the studies cited reported an improved outcome.ĭirect peritoneal resuscitation (DPR) is a resuscitation technique recently described. Recent studies have shown that gut lymph-induced lung injury can be ameliorated by low-dose albumin, sphingosine inhibition, hypertonic or hyper-oncotic resuscitation, specific neutrophil elastase inhibition or by specific inhibition of the Na +/H + exchanger presumably by mechanisms related to the detoxifying ability of the resuscitation solution, inhibition of the inflammatory signaling pathways or by modulation of white cell functions and their interaction with vascular endothelial cell. However, neither the mechanism nor the mediators of such lymph's cytotoxic effect are currently known. 
Studies on ligation of the mesenteric lymphatics suggested that nonbacterial soluble factors, generated in the gut and drained by the local lymphatics appear to be the mediator of distant organ injury. It is possible that an integral and cause-effect relationship exists between these three events to cause tissue injury and multiple organ failure. The essence of the pathogenesis of circulatory collapse due to blood loss stems from three major events 1) a persistent and progressive splanchnic vasoconstriction and hypoperfusion, 2) a gut-derived systemic inflammatory response, and 3) an obligatory fluid sequestration and failure of early mobilization. High morbidity and mortality from conventionally resuscitated hemorrhagic shock and the subsequent multiple organ failure remains a very significant and a costly clinical problem.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
